Rela Institute of Liver Disease & Transplantation is proud to have an eminent team of liver specialists, surgeons who have created a name for themselves in the field of liver surgery, treatment and transplantation.
Read More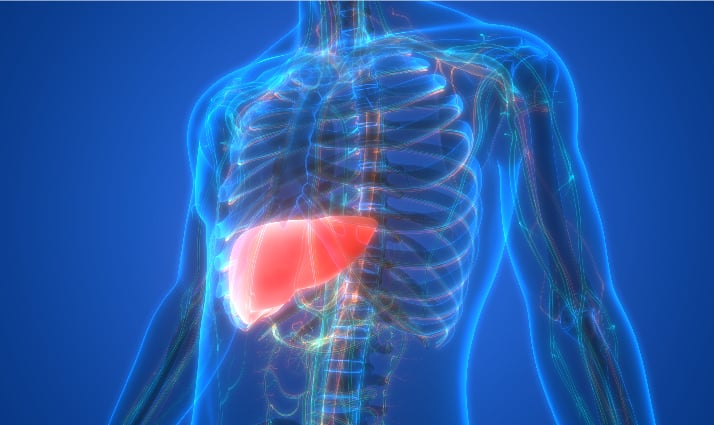
Rela Institute of Liver Disease & Transplantation (RILDT), which is the Largest Liver Centre in India and the Largest Paediatric Liver Transplant Centre in the World, is a beacon of hope where the latest medical advancements meet compassionate, patient-centered care. Our highly skilled liver specialists, nurses, and support staff are dedicated to delivering exceptional care and support to patients and their families during one of their most challenging times.
At the forefront of medical innovation, our state-of-the-art facilities and cutting-edge technologies allow us to provide the latest treatments and therapies for liver conditions. From minimally invasive surgical options to innovative medical treatments, we are dedicated to finding the best solution for each patient.
At the Rela Institute of Liver Disease & Transplantation (RILDT), we believe that a warm and supportive environment is just as important as cutting-edge medical care. That’s why our team takes a personalised approach, working closely with patients and their families to develop individualised care plans and provide emotional and psychological support throughout their journey.
Our goal is to help our patients return to the lives they love with the peace of mind that they are in the hands of the best medical professionals, which makes us one of the best liver hospitals in India.
Rela Institute of Liver Diseases & Transplantation (RILDT) performed India’s Youngest Successful Liver Transplantation on a One-Month-Old Baby.
Rela Institute of Liver Disease & Transplantation’s (RILDT) team of eminent doctors and surgeons have established some of the ‘firsts’ as their career achievements:
Over two decades, Rela Hospital has proved to be the best liver specialists for liver transplant in India. The Transplant team is entirely capable of coordinating with the patient from the moment they register themselves for a transplant to the time of complete recovery.
The care and attention we give to our patients are all-round and positive. For this reason, they go back home feeling satisfied and ready to return to their daily lives with great enthusiasm.
If you would like to acquaint yourself with our way of working and all our facilities, kindly drop in at our hospitals. For an appointment, call on +91 9384681770
Liver transplant recipients can live for many years, and the survival rates have improved significantly over the years due to advancements in medical procedures and post-transplant care. Many individuals can live for more than 20 years post-transplant, and some have even surpassed 30 years. However, individual outcomes can vary based on various factors like the recipient’s overall health, the cause of liver failure, the age of the recipient, and adherence to post-transplant medication and lifestyle recommendations.
There is no strict minimum age for a liver transplant. The eligibility for a liver transplant depends on the specific medical condition of the patient and whether they meet the criteria for transplantation. Paediatric liver transplantation is performed in infants and children with life-threatening liver diseases that cannot be managed effectively with other treatments. The decision for liver transplantation in paediatric cases is made based on the assessment by a specialised medical team that evaluates the child’s medical condition and overall health.
Thеrе arе two main typеs of livеr transplants:
Both typеs of transplants havе thеir own advantagеs and considеrations, and thе choicе bеtwееn thеm dеpеnds on thе patiеnt’s condition, availability of suitablе donors, and mеdical еvaluation.
Exact statistics on the number of people who live 20 years or more after a liver transplant might not be readily available, as it can vary over time and between different transplant centres. However, it is known that many liver transplant recipients can achieve long-term survival, and it is not uncommon for individuals to live 20 years or more after a successful transplant.
A liver transplant is a major surgery and, like any other surgical procedure, carries risks. Some potential risks and complications of liver transplant include:
It’s essential to remember that transplant teams carefully evaluate potential recipients and donors to minimise these risks and ensure the best possible outcomes.
The liver is a unique organ that can regenerate. During a liver transplant, both the donor and recipient typically receive a portion of the liver. In living donor liver transplantation, the donor donates a portion of their liver, usually the right lobe or a segment of the right lobe, which is sufficient for the recipient. The donor’s liver will regenerate to nearly its original size within a few months after surgery. In deceased donor liver transplantation, the entire liver is transplanted from a deceased donor to the recipient.
Liver rejection occurs when the recipient’s immune system identifies the transplanted liver as foreign and tries to attack it. The signs of liver rejection can vary, but some common early symptoms may include:
If any of these symptoms are noticed, the patient must inform their transplant team immediately, as early detection and prompt treatment of rejection episodes are crucial for successful long-term outcomes.
The eligibility for a liver transplant depends on the individual’s medical condition and the severity of their liver disease. In some cases, a patient’s health may deteriorate to the point where they are no longer suitable candidates for a transplant due to poor overall health, advanced age, or other medical complications. Each case is unique, and the decision regarding transplant eligibility is made by the transplant team after a thorough evaluation of the patient’s condition.
After a liver transplant, patients are usually advised to follow a healthy and balanced diet to support their recovery and overall well-being. Some general dietary recommendations may include:
However, specific dietary recommendations may vary based on individual health needs, and patients should follow the guidance provided by their transplant team or a registered dietitian.
Liver transplantation is not suitable for everyone, and eligibility criteria may vary depending on the transplant centre and the patient’s specific medical condition. Some common reasons why a patient might be considered ineligible for a liver transplant include:
Each case is evaluated individually, and the transplant team assesses the potential risks and benefits to determine if a liver transplant is the appropriate course of action.
RILDT is proud to have an eminent team of liver specialists, surgeons who have created a name for themselves in the field of liver surgery, treatment and transplantation.

We have taken measures to maintain the strength and resilience of RILDT’s core infrastructure. Additionally, we have ensured that RILDT adheres to international standards. To that end, we have
Prof Mohamed Rela is the pioneer of organ transplant care in India with expertise in liver transplants. The liver transplant program at Rela Hospital is one of the most advanced programs in the country, delivering a wide range of transplant options.
It has been nearly a decade since the inception of the Paediatric Liver Transplantation Program in Chennai by Prof. Mohamed Rela and his team! Over this period, the program has been a sterling example of progress in the field with multiple pioneering efforts in the field, saving lives and garnering accolades along the way!
Liver cancer involves malignant hepatic tumors in or on the liver. Liver cancer is a type of cancer that starts in the liver. Some cancers develop outside the liver and spread to the area. However, only cancers that start in the liver are described as liver cancer.
Cirrhosis is chronic condition of scarring the liver tissues that impairs blood supply to liver and hampers vital liver functions. Liver cirrhosis is primarily caused due to infections, hepatitis and alcohol abuse.
The liver is a robust organ of the human body, undertaking several key functions in metabolism. Liver diseases reduce the ability of the organ to undertake its functions and therefore easily compound into the disease & complications.
Chronic liver disease is one of the important causes of morbidity and mortality around the world. Excess alcohol consumption, chronic viral infection and obesity are the leading causes of chronic liver disease
Acute Liver Failure (ALF) refers to a severe failure of liver function within a matter of days to weeks in a previously healthy person. Acute liver failure is less common than chronic liver failure, which develops more slowly. The most common cause of ALF in India is viral infection due to hepatitis viruses. Other causes of ALF include:
Occasionally a patient may need transplantation of both the liver and kidney together. This can be because the patient has both liver and kidney failure or occasionally when the liver problem is causing the kidneys to fail (as in hyperoxaluria)
RILDT is considered the best hospital for liver cancer in Chennai and has one of the highest liver cancer survival rates. We are good because we identify liver tumors, which usually do not present with any specific symptoms until they are large in size.
Cholangiocarcinoma refers to tumor involving the bile duct. Patients with this disease present with jaundice, itching and pale coloured stools. Early diagnosis of this tumor is the key to good outcome as complete surgical removal of this tumor gives the best long-term outcomes.
Acute Pancreatitis is an inflammation of the pancreas of sudden onset that is short-lived and usually resolves over a period of time. It is most commonly caused by alcohol abuse or gallstones.
Let’s explore non-alcoholic fatty liver disease (NAFLD): Non-alcoholic fatty liver disease is characterized by accumulation of fat in the liver.
Alcoholic Liver Disease (ALD), also known as Alcohol-Related Liver Disease (ARLD) is a medical condition that often comprehends various liver related conditions, primarily associated with the overconsumption of alcohol.
When the stomach has an abnormal build-up exceeding 25 millilitres of fluid, the condition is known as Ascites. This condition arises when the liver ceases to function normally. In such a situation, fluid takes up the space between the organs and the abdominal lining.
Hepatitis B is a viral infection of the liver due to Hepatitis B virus (HBV). In some individuals the viral infection is acute and can be resolved with immediate medical attention, where as in some cases infection is chronic and lasts for months.
Hepatitis C is a viral infection of liver causing redness and inflammation. Hepatitis C virus (HCV) spreads through inflected blood from one person to another. Weekly Injection and medications is advised to cure the patient.
Hepatic encephalopathy is diagnosed as a reduction in brain functioning that is caused by chronic liver disease. Patients of hepatic encephalopathy have poorly functioning livers that are not equipped to remove any toxins in the blood.
Wilson’s disease is a genetic disorder affecting people from 3 – 55 years of age. Wilson’s disease is identified by copper toxicity in diverse body tissues, liver, brain, corneas of the eyes and other vital organs.
Chronic liver disease is defined as when symptoms of liver disease like jaundice, tiredness, abdominal distention, leg swelling, vomiting blood or altered behaviour are present for more than 6 months.
At RILDT, we are one of the very few liver units in the country having the ability to manage sick patients and undertake liver transplantation on an emergency basis.
Doctors in the Division of Hepatopancreatico Biliary surgery form a diverse team of deeply experienced specialists to care for people with Liver , Pancreas and Gall Bladder disorders.
Your biliary tract, which is made up of your gallbladder and bile ducts, helps with digestion by releasing bile.The gallbladder is a pear-shaped organ that sits just below your liver on the upper right side of your abdomen.
A gallbladder polyp is a small, abnormal growth of tissue with a stalk protruding from the lining of the inside of the gallbladder. They are relatively common.The gallbladder is a small organ that stores bile and passes it from the liver to the small intestine.
Choledocholithiasis (also called bile duct stones or gallstones in the bile duct) is the presence of a gallstone in the common bile duct. Gallstones usually form in your gallbladder.
Liver metastasis is also known as secondary liver cancer or stage IV cancer of the liver. In this condition the cancer spreads to the liver which originated in another part of the body.
Inflammation in the bile duct system causes Cholangitis. The bile duct system is responsible for carrying bile from the liver and gall bladder into the duodenum.
The disease, Primary Biliary Cholangitis (PBC) or Primary Biliary Cirrhosis results when the liver’s bile ducts are damaged. Through these outlets, bile pours into the small intestine. Here, bile breaks down fats and helps absorbing vitamins soluble by fat. It also absorbs other vitamins.
An enlarged liver or one that is much larger than normal is called Hepatomegaly. There are several causes of liver enlargement, so the term “Hepatomegaly” does not refer to a specific disease but to a range of conditions.
A rare congenital disease among children, Crigler-Najjar Syndrome is identified by a substance that the liver processes called bilirubin. It cannot be altered to its water-soluble state or conjugated bilirubin.
A congenital disorder, Galactosemia affects the way the body processes galactose, a simple sugar. Some babies are born with this disorder that prevents their systems from processing galactose by drinking breast milk and formula. Ordinarily, this gets converted into energy, but not for those babies who cannot process it easily.
A rare condition that affects just one in every million adults, Budd-Chiari syndrome results due to blood clots that partially or completely block blood flow out of the liver
A rare and benign liver tumour, Liver or Hepatic Adenoma is also called hepatocellular adenoma or liver cell adenoma. It usually affects women and is said to be caused due to birth control pills.
Cancer that originates in the liver is called Hepatocellular Carcinoma. This makes it different from other secondary liver cancers that originate in other organs and then spread to the liver. If detected early, Hepatocellular Carcinoma can be cured either with a liver transplant or surgery.
Hepatoblastoma is a kind of liver cancer that usually shows up in babies and little children not older than three years. This is a very rare type of cancer that originates in the liver and doesn’t spread to other body parts. It usually first shows up in the right ear lobe and, if it spreads, you can see it next in the lungs.
A life-threatening condition and progressive type of kidney failure, it is commonly seen in those with acute liver damage. Usually, cirrhosis is the cause of Hepatorenal Syndrome (HRS). Apart from cirrhosis, ascites is also a cause of this condition just as fulminant hepatic failure is.
The portal vein carried blood from the digestive organs such as the stomach and pancreas to the liver. When an increase in pressure in this vein is seen, portal hypertension sets in. Cirrhosis of the liver and thrombosis are the most common causes of this.
A liver hemangioma is a benign lump of blood vessels either in the liver or on its surface. This tumour doesn’t cause any symptoms. In fact, most people don’t even know they have a liver hemangioma.
The surgical removal of a part or whole of the liver is termed liver resection. This surgery is performed when a diseased liver is removed from a cadaver or a liver transplant takes place.
The success rate of a liver transplant is generally very high, with most patients recovering well and leading healthy lives after the procedure. The outcome depends on factors like the type of donor, the overall health of the patient, and adherence to post-transplant care, especially taking prescribed medications to prevent rejection. With proper medical support and follow-up, liver transplant recipients can enjoy a good quality of life.
Generally, patients receiving fresh new livers lead a normal and healthy life post-surgery. The first three months after surgery are critical because the patient must observe the doctor’s rules while the liver is adjusting to his system.
At Rela Hospital, one of the best liver transplant hospitals in Chennai, India, doctors insist that patients take the medications as prescribed for best results. When patients are discharged, they show that they can look after themselves and this lengthens their lifespan and promotes a better quality of life with few, if any, complications.
Liver disease could recur; Hepatitis C is one of them. Should the patient display any changes in the patient, the transplant team will help prevent any further liver ailments from damaging the new liver. The patient too should be careful of not contracting any ailment.
Yes, the patient will experience a significant amount of pain post-surgery. Of these, those with stomach surgeries will experience more pain because of the abdominal incision that causes the skin to turn numb in the abdominal region. In the months following the surgery, a patient could experience pain in this region due to the regrowth of nerves.
Another possible side-effect is back pain due to the number of hours the patient spends on the operating table.
However, this pain will gradually decrease through recovery, and can also be dealt with to a certain extent through prescribed dosages of painkillers.
An incision is made from the right part of the mid-section reaching the ribs. It also goes as far as the left part of the stomach. This is better known as the “Chevron Incision”. This cut is also made from the breast bone to the horizontal cut. This cut is therefore large and will bring about pain, with a scar that remains.
After the transplant surgery, patients are kept in hospital for 10 days so that doctors can check for any issues after surgery. They also check the patient’s rate of recovery. Once the doctor is sure the patient is recovering well, he will be discharged, according to the best liver transplant surgery doctors in Chennai, India. After three months, they can get back to work and lead a normal life.
Crigler-Najjar Syndrome: Symptoms, Diagnosis, and Treatment Options

Importance of MELD Score in Liver Transplantation
April 26, 2025
All About Becoming a Liver Donor
April 26, 2025

Hepatoblastoma in Children: Causes, Symptoms, Diagnosis, and Treatment
April 24, 2025

All About Non-Alcoholic Fatty Liver Disease
November 12, 2019












