Celiac Disease: Causes, Symptoms, and Diet Tips
April 13, 2026
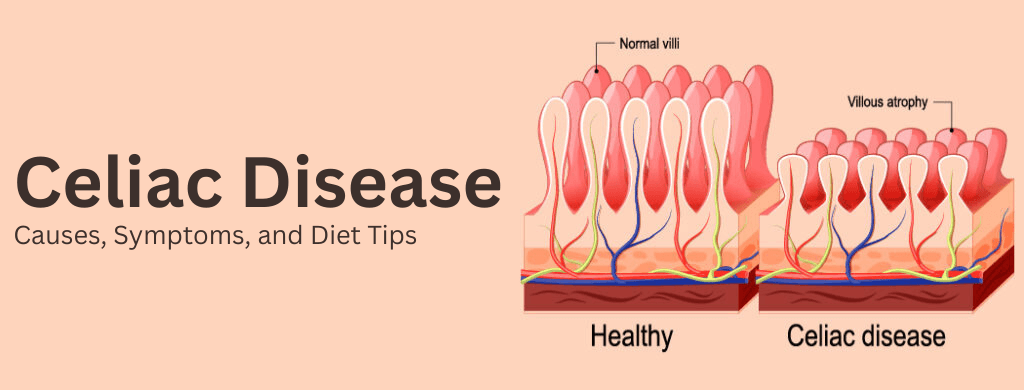
Celiac disease is a digestive disorder that harms the small intestine when gluten is consumed. Wheat, barley, and rye contain this protein, which triggers the condition. You should remove gluten from your diet to alleviate symptoms and support healing. Gluten consumption in people with celiac disease causes their immune system to mistakenly target and damage the small intestine. This damages the villi, which are tiny finger-like projections that help absorb nutrients. Consequently, the body has difficulty absorbing vital nutrients. This can lead to malnutrition, weakened bones, infertility, miscarriage, neurological disorders, or even certain types of cancer.
If symptoms persist for over a year despite following a strict gluten-free diet, doctors may diagnose refractory or nonresponsive celiac disease. Many people with celiac disease remain undiagnosed because symptoms vary widely, and the damage occurs slowly over time. It is important to note that gluten sensitivity or intolerance differs from celiac disease. While both can cause similar digestive symptoms, gluten intolerance does not trigger an immune response or damage the small intestine. However, people with gluten sensitivity may still choose to avoid gluten to feel better.
The signs of celiac disease are distinct from those of a food allergy. Eating wheat with a wheat allergy can make breathing hard or cause itchy, watery eyes.
Symptoms
Symptoms in Adults
Adults who have celiac disease could have digestive issues. However, symptoms frequently spread to other parts of the body. These signs could consist of the following:
- Iron-deficiency anaemia
- Painful and stiff joints
- Brittle and fragile bones
- Fatigue
- Skin disorders
- Tingling and numbness in the hands and feet
- Loss of enamel or tooth discoloration
- Pale mouth sores
- Irregular intervals of menstruation
- Miscarriage and infertility
Another typical sign of celiac disease is dermatitis herpetiformis (DH). DH is a bumpy, blistering skin rash that itches terribly. It might appear on the knees, buttocks, and elbows. About 15 to 25% of people living with celiac disease also have DH. Those who do have DH typically don’t have any intestinal issues.
It’s crucial to remember that symptoms might differ from person to person depending on several circumstances, such as:
How long a person was breastfed when they were little, when they first started consuming gluten, and the amount of intestinal damage depend on how much gluten is consumed.
Some people living with celiac disease don’t exhibit any symptoms. However, they still risk getting long-term repercussions from their illness.
Symptoms in Children
- Nausea and vomiting
- Chronic diarrhea
- Swollen belly
- Constipation
- Gas
- Pale, foul-smelling stools
If you think you or your kid may have celiac disease, book an appointment with your doctor. Complications are more likely to develop when diagnosis and treatment are delayed.
Causes
According to research, individuals with celiac disease have specific genes and can only consume gluten-containing foods. People with one of the two groups of common gene variations, known as DQ2 and DQ8, nearly always get celiac disease. It is improbable that those without these gene variations will get celiac disease. DQ2 or DQ8 is present in about 30% of the population. Only 3% of those with DQ2 or DQ8 go on to develop celiac disease, though. Other genes that may raise the risk of celiac disease in people with DQ2 or DQ8 are being researched.
Risk Factors
Celiac disease can affect anyone, but some people have a higher chance of developing it. These are called risk factors.
1. Family History
If someone in your close family has celiac disease, your risk is higher. This includes parents, brothers, sisters, or children. Genetics play an important role in this condition.
2. Gender
Celiac disease is more common in women than in men. Women are more likely to be diagnosed with this condition.
3. Other Autoimmune Diseases
People who already have autoimmune diseases have a higher risk. These include:
- Type 1 diabetes
- Thyroid disorders
- Addison’s disease
In these conditions, the immune system attacks the body, just like in celiac disease.
4. Genetic and Chromosomal Conditions
Certain genetic conditions can increase the risk, such as:
- Down syndrome
- Turner syndrome
- Williams syndrome
These conditions are linked to changes in chromosomes.
5. Skin Condition Linked to Celiac Disease
People with a skin condition called dermatitis herpetiformis are more likely to have celiac disease. This condition causes itchy skin rashes.
6. Other Related Conditions
Some other health problems may also increase the risk, such as:
- Microscopic colitis
- Certain digestive disorders
Diagnosis
Celiac disease can be difficult to identify because its symptoms often resemble those of other digestive conditions. Many people do not even know they have it. Doctors use a step-by-step approach to confirm the condition.
1. Medical History and Physical Exam
The doctor will first ask about your symptoms, eating habits, and family history. They may also do a simple physical check to look for signs like weight loss or weakness.
2. Blood Tests
Blood tests are usually the first step. These tests check for special proteins called antibodies. These antibodies increase when your body reacts to gluten.
It is important to keep eating gluten before the test. If you stop eating gluten, the results may appear normal even if you have the disease.
3. Genetic Testing
Doctors may also check for certain genes (HLA-DQ2 and HLA-DQ8). If these genes are not present, celiac disease is very unlikely. This test helps rule out the condition.
4. Endoscopy and Biopsy
If blood tests suggest celiac disease, doctors may do an endoscopy. In this test, a thin tube with a small camera is passed through your mouth into the small intestine.
The doctor takes a small tissue sample (biopsy) from the intestine. This sample is checked for damage. Damage to the intestinal lining confirms celiac disease.
5. Capsule Endoscopy
In some cases, you may swallow a small capsule with a camera inside. It takes pictures of your small intestine as it moves through your body. This helps doctors see areas that are hard to reach.
6. Additional Tests
After diagnosis, doctors may do more tests to check your overall health. These may include:
- Blood tests to check for anemia
- Vitamin and mineral levels
- Liver function tests
- Bone density scan to check bone health
Important Note
Celiac disease symptoms can look like other conditions such as irritable bowel syndrome or food intolerance. That is why proper testing is important. Always consult a doctor for an accurate diagnosis.
Diet Tips to Follow
Most people with celiac disease find that being gluten-free dramatically reduces their symptoms, and they can start to feel better in a matter of days or weeks. The small intestine often recovers in children in 3-6 months. Full recovery can take several years in adulthood. However, the body can more adequately absorb nutrients from meals after the intestines have healed. If you have celiac disease, it’s essential to remove all gluten-containing foods and drinks from your diet. Following a gluten-free diet helps relieve symptoms and promotes healing of the small intestine. You can get advice on what to eat and drink to keep a balanced diet from your doctor or a qualified dietitian. Always check with your doctor regarding your diet and food intake. Below are a few suggestions on what to consume and what not to eat.
What to Consume:
Wheat, rye, and barley are natural sources of gluten. Gluten is also found in most grains, pasta, and processed meals, as well as beers and other alcoholic beverages made from grains. Because gluten can be an element in unexpected items, it is important to read labels carefully.
The following foods don’t contain gluten:
- Meat, fish, poultry
- Eggs
- Fruits and vegetables
- Some grains, like rice, amaranth, quinoa, and buckwheat; rice flour cereals, such as corn, millet, sorghum, and teff; and gluten-free pasta, bread, baked goods, and more.
What Not to Consume:
Additionally, gluten can be removed from recipes by substituting and, in some cases, modifying the baking time and temperature. The following list of processed foods may contain gluten:
- Canned soup
- Salad dressings
- Ketchup
- Ice cream, seasonings, candy bars, and soy sauce
- prepared meats and sausages in cans
Gluten is present in various non-food products, including toothpaste, lipstick, lip balm, lip gloss, and postage stamps.
The key to managing celiac disease is strictly avoiding gluten at all times. Following the diet carefully helps reduce symptoms and protects your intestine from damage.
Complications
If celiac disease is not properly managed, it may cause several health issues over time.
- Malnutrition: The body cannot absorb enough nutrients, leading to weight loss, weakness, and anemia.
- Weak bones: Low calcium and vitamin D can cause soft or fragile bones.
- Digestive issues: Problems like bloating, diarrhea, and lactose intolerance may occur.
- Reproductive problems: It may lead to infertility or miscarriage.
- Nerve problems: Some people may feel tingling, numbness, or balance issues.
- Liver issues: It can affect liver function in some cases.
- Cancer risk: Untreated celiac disease may increase the risk of certain cancers (rare).
Maintaining a strict gluten-free diet can help reduce the risk of most of these complications.
Whom Should I Consult?
If you have celiac disease, your doctor or gastroenterologist can offer ongoing care and support. If blood tests or an endoscopy do not detect celiac disease, you are unlikely to have the condition. However, other diseases can cause similar symptoms. A gastroenterologist can help find the underlying cause of your symptoms.
Before starting a gluten-free diet, consult your healthcare team. Reducing or eliminating gluten before testing can affect the accuracy of your results. Celiac disease often runs in families. If a family member has celiac disease, consult your healthcare provider to determine if you should get tested. You should also consider testing if you or a relative has a risk factor, such as type 1 diabetes.
Frequently Asked Questions
1. What is the life expectancy of a person with celiac?
Celiac disease is not directly fatal, but it may slightly increase the risk of premature death from conditions like cardiovascular disease, cancer, and respiratory diseases. However, following a strict gluten-free diet can significantly lower this risk.
2. Can celiac disease be cured?
There is no cure for celiac disease, but maintaining a strict, lifelong gluten-free diet can effectively manage symptoms, promote small intestine healing, and prevent long-term complications.
3. How is Non-Celiac Gluten Sensitivity Different from Celiac Disease?
Celiac disease harms the small intestine. Blood tests detect specific markers that help confirm the diagnosis. Non-celiac gluten sensitivity causes symptoms such as brain fog, nausea, vomiting, migraines, diarrhea, joint pain, and abdominal discomfort. Unlike celiac disease, NCGS does not damage the intestine. Doctors diagnose NCGS by observing symptom improvement after following a gluten-free diet.
4. Can Celiac Disease Cause Weight Gain?
When someone with celiac disease begins a gluten-free diet, weight gain is frequently the result. It actually indicates that the gut lining is healing. However, additional health issues, such as heart disease and high blood pressure, might develop if weight gain persists and results in becoming overweight.






