Non-alcoholic Fatty Liver: Symptoms, Causes and Treatment
November 5, 2019
At least 30% of the Western population is estimated to have Non-alcoholic fatty liver disease (NAFLD). It is the commonest cause of abnormal liver tests in the community and is closely associated with his ‘big brother’ Metabolic Syndrome (MS), which comprises central obesity, type 2 Diabetes Mellitus (type 2 DM), hypertension and hyperlipidemia.
NAFLD may be present in at least 50-70% of patients with type 2 DM. India being the ‘diabetic capital’, one would anticipate a much higher prevalence of NAFLD. In patients with NAFLD, the prevalence of MS is around 40%. NAFLD is emerging as an important health issue of concern in both adults and children because it increases the risk of type 2 diabetes mellitus, hypertension, ischaemic heart disease and death.
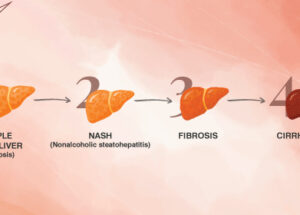
NAFLD, the liver manifestation of MS is characterized by steatosis (fatty liver). Progressive steatosis leads to non-alcoholic steatohepatitis (NASH) in at least 40% of patients, which is characterized by hepatic inflammation. Long-standing inflammatory milieu leads to fibrosis and eventually to approximately 10% of patients. Studies show that many cases of ‘cryptogenic cirrhosis’ is probably due to ‘burnt out’ NASH.
In addition, NASH cirrhosis increases the risk of hepatocellular carcinoma by several folds. The presence of diabetes increases the risk of fibrosis. In addition, obesity also results in progressive liver damage leading to cirrhosis.
Symptoms of Non-alcoholic Fatty Liver
Like most chronic liver conditions, patients with NAFLD are asymptomatic until late. The majority of them are detected rather incidentally. If you do have symptoms, they may include:
- Abdominal Pain
- Nausea or loss of appetite
- Jaundice
- Swollen abdomen and legs
- Extreme tiredness
- Weakness
Causes of Non-alcoholic Fatty Liver
Some people get fatty liver disease without having any pre-existing conditions, some causes include
- Genetic Inheritance
- Obesity
- Rapid weight loss
- Diabetes
- Fats in the blood
- Side effects of medications
Pathogenesis of NAFLD steatosis
The pathogenesis of NAFLD is complex. There is wary of metabolic imbalance in adipocytes and the liver. Increased intake of carbohydrate and fructose-containing diet results in hyperinsulinemia. This results in adipose tissue insulin resistance, which subsequently causes lipolysis resulting in increased FFA. This FFA is utilized for hepatic triglyceride synthesis resulting in steatosis. In the liver, hepatic insulin resistance and increased dietary carbohydrates result in lipogenesis.
Steatohepatitis
Hyperlipidemia and hepatic steatosis activate proinflammatory cytokines TNF alpha secreted by activated Kupffer cells through mitochondria dysfunction, lysosomal disruption and endoplasmic reticulum (ER) stress resulting in steatohepatitis. Chronic liver injury results in hepatocyte death.
Fibrosis and cirrhosis
Chronic inflammation and reduced adiponectin stimulate stellate cells resulting in scarring (fibrosis). Reduced Persistent fibrosis leads to the development of cirrhosis.
Treatment of Non-alcoholic Fatty Liver
Measures to improve insulin sensitivity is the key for both NAFLD and MS management. However, the lack of single effective therapy led to multi-dimensional treatment approaches such as lifestyle modification, weight loss, change in dietary habits and exercise. Weight loss of 5-10% over 6 months has been shown to improve NAFLD and indeed obesity. Rapid weight loss ironically exacerbates NAFLD and hence is not recommended.
-
- Diet
Diet and exercise are shown to reduce hepatic steatosis and obesity. Diet rich in carbohydrates and saturated fats should be avoided. Most fast food contains trans-fat that has been shown to worsen liver injury and increase hepatic triglycerides. Polyunsaturated fatty acids seem to improve liver enzymes. Many soft drinks contain fructose that increases lipogenesis, insulin resistance and NAFLD. Hence, excessive soft drinks are generally not recommended. Diet with a low glycemic index, rich in fruits & vegetables with limited meat consumption is recommended.
-
- Exercise
Exercise aids weight reduction, improvement in liver enzymes and decreases the risk of type 2 DM. Moderate exercise with the expenditure of 400 calories at least 3-4 times a week has been shown to improve NAFLD in the short term.
-
- Drugs
Various drugs have been studied with varying results.
-
-
- Metformin is an insulin-sensitizing agent. Apart from improving insulin sensitivity, it helps weight reduction. When used for NAFLD patients there was some reduction in liver enzymes, however, randomized controlled studies showed no improvement in liver histology.
- Pioglitazone increases insulin sensitivity, improves steatosis, and inflammation. However, it is associated with weight gain. Rosiglitazone improves liver histology (FLIRT trial) but only in the short term but not in the long term. This drug has been suspended by the FDA due to cardiovascular risks.
- Orlistat is a lipase inhibitor. Studies show that it improves transaminases, steatosis and weight reduction of 8% over 3 months. Long term studies are required to confirm its benefit. Side effects are bloating and diarrhoea.
- Sibutramine is a serotonin reuptake inhibitor that increases satiety leading to moderate weight reduction. This drug has been withdrawn from the UK due to cardiovascular risks.
- Rimonabant is a cannabinoid receptor antagonist which was shown to improve insulin sensitivity but this drug was withdrawn from the market due to severe psychiatric effects.
- A new glucagon-like peptide (GLP-1) analogue, Exanetide has been studied. In patients with type 2 DM, it has been shown to improve glycemic control, suppress appetite and also induces weight reduction. This may be beneficial in patients with MS and NAFLD in the future.
- Angiotensin receptor blocker (ARB) such as Losartan has been shown to inhibit proinflammatory cytokines and stellate activation. Human studies in small numbers showed improved liver enzymes and histology in NASH patients. Long term data is not available.
- Pentoxyphylline, Vitamin E and UDCA failed to show any benefit in NAFLD patients.
- Surgery
-
Bariatric surgery has been increasingly performed throughout the world. A recent meta-analysis suggested improvement in steatosis and steatohepatitis of 90% and 80%, respectively, but the varying outcomes on fibrosis. Various options include Roux-en Y gastric bypass, laparoscopic gastric banding. It should be considered for morbidly obese (BMI>40) patients who are otherwise unable to lose weight by other measures.
Endoscopically placed Intragastric Balloon (IB) is an attractive alternative to bariatric surgery. This is a temporary measure that has been shown to improve liver enzymes, insulin sensitivity if the weight reduction was >10%. Long term data is needed to confirm its efficacy.