Amyloidosis: Causes, Types, Symptoms, and Treatments
August 4, 2025
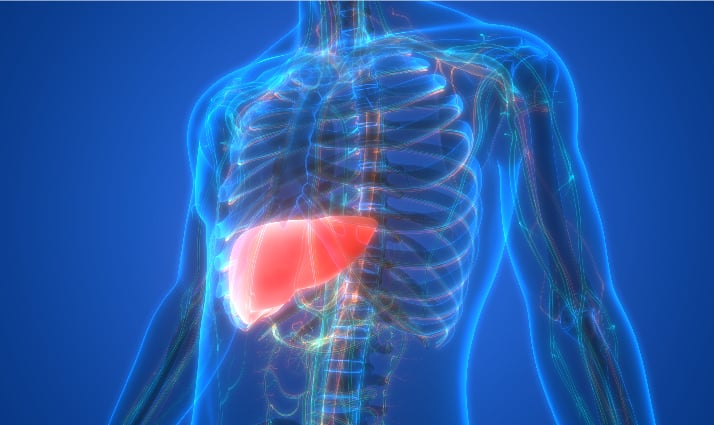
Amyloidosis is a condition that occurs when amyloid, an abnormal protein, accumulates in your tissues and organs. When this happens, it affects their shape and how they function. A person might have amyloidosis in one or many organs.
Causes
A lot of proteins can lead to amyloid deposits in your body, but very few of them have been linked to severe health problems. The type of protein and where it is deposited will define the kind of amyloidosis that you might possess.
Types
Amyloidosis is classified into different types based on the specific protein involved and the underlying cause.
1. AL Amyloidosis (immunoglobulin light chain amyloidosis)
This is the most prevalent kind and was previously known as primary amyloidosis. AL stands for “amyloid light chains,” the sort of protein that causes the illness. The condition arises from the bone marrow generating faulty antibodies that the body is unable to eliminate, though its exact cause remains unclear. It has been related to multiple myeloma, a kind of blood cancer. It can potentially damage vital organs such as the kidneys, heart, liver, intestines, and nerves.
2. AA Amyloidosis
Previously referred to as secondary amyloidosis, this disorder is triggered by chronic infectious or inflammatory conditions like rheumatoid arthritis, Crohn’s disease, or ulcerative colitis. Although it can have an impact on the digestive tract, liver, and heart, it primarily affects the kidneys.
3. Dialysis-related Amyloidosis (DRA)
This is especially common in the elderly and those who have been on dialysis for more than five years. This form of amyloidosis results from the buildup of beta-2 microglobulin deposits in the bloodstream. Deposits can form in various tissues, but bones, joints, and tendons are the most common.
4. Familial, or Hereditary, Amyloidosis
This is an uncommon variant that is passed down via families. It commonly impacts the liver, nerves, heart, and kidneys. Numerous genetic mutations have been associated with a higher risk of developing amyloidosis. An aberrant protein, such as transthyretin (TTR), could be the reason.
5. Age-related (Senile) Systemic Amyloidosis
This is due to typical TTR deposits in the heart and other tissues. It mostly affects older men.
Organ-specific amyloidosis
This results in amyloid protein accumulation in individual organs, including the skin (cutaneous amyloidosis).
Though some amyloid deposits have been related to Alzheimer’s disease, amyloidosis, which occurs throughout the body, seldom affects the brain.
Types Based on the Different Organs of Our Body
Amyloidosis can affect various organs, leading to distinct types based on where abnormal protein deposits accumulate. Below are the major types categorized by the organs they impact.
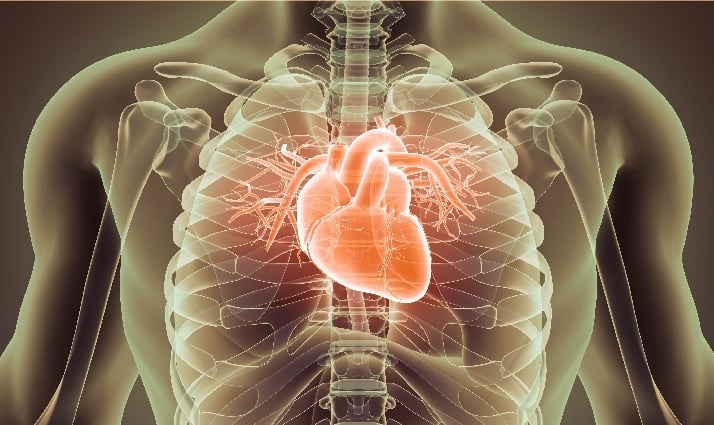
1. Cardiac Amyloidosis
Amyloid deposits in the heart can stiffen the heart muscle walls. They can also weaken the heart muscle and disrupt its electrical rhythm. This disorder may result in a reduced blood supply to your heart. Over time, your heart may lose its ability to pump effectively. If you happen to have cardiac amyloidosis, you will experience the following symptoms:
- Breathing difficulties with light activity
- An unsteady heartbeat
- Heart failure symptoms include swelling of the feet and ankles, weakness, weariness, and nausea.
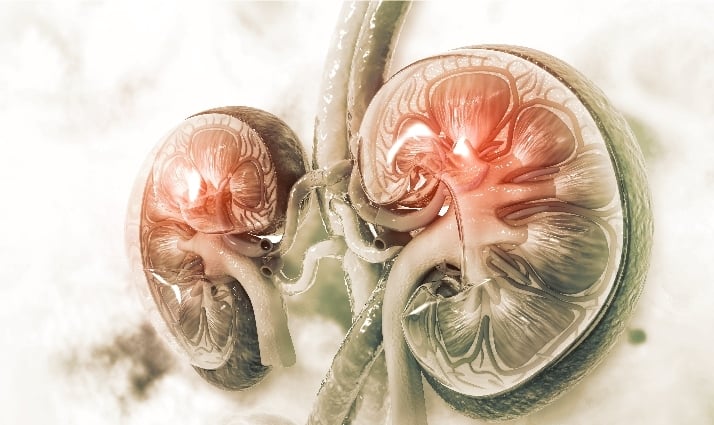
2. Renal Amyloidosis
Your kidneys are responsible for filtering waste and poisons from your blood. However, amyloid deposits in the kidneys make it difficult for them to perform this function. When your kidneys fail to function properly, water and hazardous poisons accumulate in your body. People with renal amyloidosis will experience the following symptoms:
- Signs of renal failure include swelling of the feet and ankles and puffiness around the eyes.
- Protein levels in your urine will be high.
3. Gastrointestinal Amyloidosis
Amyloid deposits in your GI tract slow down the flow of food through your intestines. This obstructs digestion. If amyloidosis affects your GI tract, the following symptoms will be experienced:
4. Amyloid Neuropathy
Amyloid deposits can harm the peripheral nerves, which are the nerves that run outside of your brain and spinal cord. Peripheral nerves connect your brain and spinal cord to the rest of your body. For example, burning your fingers or stubbing your toes causes your brain to sense pain. When amyloidosis affects your nerves:
- Balancing problems
- No control over your bowel movements
- Sweating problems
- Tingling and weakness
- Lightheadedness when standing due to an issue with your body’s ability to control blood pressure
Risk Factors
Multiple factors can contribute to the risk of developing amyloidosis. While some risks are inherited, others stem from chronic conditions or long-term medical treatments. Below are the key risk factors:
Ethnicity-Linked Genetic Mutations: Individuals of African descent are more likely to inherit genetic mutations linked to transthyretin (ATTR) amyloidosis, which mainly impacts the heart.
Advancing Age: The likelihood of developing amyloidosis increases with age, with most diagnoses occurring in individuals over 60.
Gender Predisposition: Men are generally more susceptible to amyloidosis compared to women.
Genetic Factors: Certain hereditary forms of amyloidosis are passed down through families, increasing the risk for those with a genetic predisposition.
Chronic Inflammatory Diseases: Prolonged inflammation from conditions like rheumatoid arthritis, Crohn’s disease, and tuberculosis can cause secondary amyloidosis (AA amyloidosis).
Multiple Myeloma Connection: A significant percentage of individuals diagnosed with AL amyloidosis also have multiple myeloma, a type of blood cancer.
Long-Term Dialysis: In cases of kidney failure, prolonged dialysis can sometimes lead to amyloid deposits, as dialysis may not efficiently remove large proteins from the bloodstream. However, modern dialysis techniques have reduced this risk.
Symptoms
Amyloidosis symptoms are frequently inconspicuous. They can also differ significantly depending on where the amyloid protein accumulates in the body. It is crucial to remember that a range of medical issues could cause the symptoms described below. A doctor can only diagnose amyloidosis.
A few general symptoms of amyloidosis are:
- Changing skin color
- Fatigue
- Severe joint pain
- Anaemia
- Falling short of breath
- The feeling of numbness and tingling in the feet and legs
- Hand grip issues
- Rapid weight loss
- Swelling in the legs, ankles, feet, or belly
Diagnosis
A comprehensive physical exam and a complete and accurate medical history are critical in assisting your doctor in diagnosing amyloidosis. Abnormal proteins can be detected using blood and urine tests. Your doctor may also examine your thyroid and liver, depending on your symptoms.
Your doctor will perform a biopsy to confirm the diagnosis of amyloidosis and determine the precise type of protein you have. The biopsy sample may be taken from abdominal fat (fat pad), bone marrow, or, in rare instances, from areas like the mouth, rectum, or other organs. It is not always necessary to do a biopsy on the area of the body affected by amyloid deposits.
Treatment
Amyloidosis cannot be cured, but your doctor may suggest treatments to slow amyloid protein buildup and help manage symptoms effectively. If amyloidosis is linked to another disorder, treatment will focus on the underlying condition.
Treatment options vary depending on the kind of amyloidosis and the number of organs affected.
- In some people with primary AL amyloidosis, high-dose chemotherapy combined with a stem cell transplant can help eliminate the chemical that causes amyloid production. Other patients with primary AL amyloidosis may be treated alone with chemotherapy medications.
- Secondary (AA) amyloidosis is treated by treating the underlying illness and using powerful anti-inflammatory medications known as steroids to combat inflammation.
- You may benefit from a liver transplant if you have certain types of hereditary amyloidosis.
- TTR production can be slowed using new medicines.
- Your doctor may also suggest a kidney transplant.
Complications
Amyloidosis can cause serious problems when abnormal protein builds up in different organs.
- Heart problems: Amyloid deposits can make the heart stiff and reduce its ability to pump blood properly. This may lead to shortness of breath, fatigue, swelling, and irregular heartbeat. In severe cases, heart complications can become life-threatening.
- Kidney damage: The condition can affect the kidneys’ filtering function. This may cause protein loss in urine, fluid buildup, and, over time, kidney failure.
- Nerve damage (neuropathy): Amyloidosis can injure the nerves, leading to pain, numbness, tingling, and weakness in the hands and feet. Some people may also have balance problems.
- Digestive and autonomic issues: Nerve involvement may disturb digestion and bowel function, causing nausea, diarrhea, constipation, or loss of bowel control. It can also affect blood pressure, leading to dizziness or fainting when standing.
- Other nerve-related symptoms: Changes in sweating, sexual dysfunction, and general weakness may occur due to damage to the autonomic nervous system.
Early diagnosis and proper treatment can help reduce the risk of these complications and improve quality of life.
Frequently Asked Questions
1. How to prevent amyloidosis?
Amyloidosis is generally not preventable, but taking steps to manage certain health conditions may help reduce the risk. Proper management of kidney disease can potentially delay or prevent kidney failure.
For AA amyloidosis, promptly treating chronic inflammatory conditions and managing inflammation effectively may lower the risk of developing the disease. For individuals with familial Mediterranean fever, healthcare professionals may prescribe colchicine to manage inflammation and help prevent AA amyloidosis.
2. When to suspect amyloidosis?
Suspect amyloidosis in unexplained fatigue, weight loss, heart failure with preserved ejection fraction, peripheral neuropathy, renal dysfunction, or multisystem involvement. Key signs include carpal tunnel syndrome, nephrotic proteinuria, macroglossia, and easy bruising.