Deep Brain Stimulation (DBS): Procedure, Benefits, and Key Facts
March 5, 2026
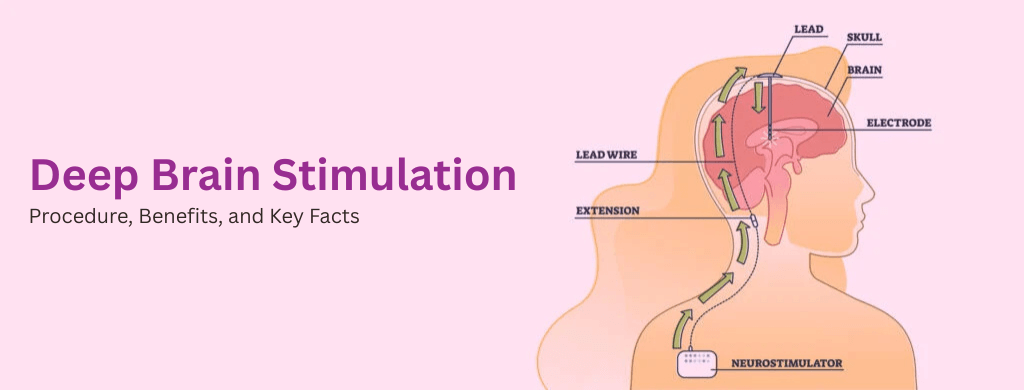
Deep brain stimulation (DBS), a well-established elective surgical method, is most commonly used to treat mental illnesses such as obsessive-compulsive disorder and movement disorders such as essential tremor, Parkinson’s disease, and dystonia. When medication fails to control a patient’s symptoms, DBS is often considered.
During surgery, electrodes are placed in specific areas of the brain. These electrodes regulate abnormal brain activity and resolve chemical imbalances, resulting in moderate electrical impulses that improve the functionality of specific brain regions. Impulses are delivered by wires connected to a programmable generator implanted beneath the skin around the collarbone.
DBS is a tremendously versatile treatment, and studies are constantly being undertaken to see if it might help with various other conditions.
5 Must-Know Facts about Deep Brain Stimulation
1. Why is DBS used?
Deep Brain Stimulation (DBS) is a surgical method in which implanted electrodes deliver precise, low-level electrical currents to modulate abnormal neuronal activity in specific brain regions. This electrical stimulation helps restore normal circuit activity in a range of neurological and mental problems. When used to treat movement disorders such as essential tremors, Parkinson’s disease, and dystonia, DBS has been proven to be particularly effective at reducing tremors, stiffness, and poor motor control.
DBS is used to treat movement disorders as well as refractory epilepsy, and it helps patients who do not respond to traditional treatments by reducing the frequency and severity of seizures. DBS can help persons with obsessive-compulsive disorder (OCD) overcome severe, intrusive thoughts and compulsive behaviours that impair their daily lives.
Patients who have not received adequate symptom alleviation from medications or other non-invasive treatments will benefit most from this operation. Although the specific mechanism of the DBS effect is still being investigated, it is considered to help restore balance within neural circuits by altering the activity of hyperactive or underactive brain locations. Because the therapy is reversible and adaptable, medical experts can adjust the stimulation parameters to optimise each patient’s results.
2. How does DBS work?
Deep brain stimulation (DBS) is a highly sophisticated surgical technique that involves placing small, insulated electrodes into specific brain locations. These areas were chosen because they are involved in the symptoms of specific mental or neurological illnesses. The implanted electrodes deliver continuous, low-level electrical impulses, or “shocks,” which interact with the brain’s electrical signals. This stimulation improves the functionality of damaged areas while also reducing symptoms by regulating abnormal neural activity.
A tiny, battery-powered gadget known as a pulse generator is inserted beneath the skin close to the collarbone to produce electrical impulses. Because the pulse generator is programmable, medical professionals can alter the stimulation’s frequency, strength, and duration to meet the demands of each patient. Because it allows for continuous therapeutic optimisation to maximise efficacy while minimising potential side effects, this flexibility is essential.
The particular mechanisms of DBS activity are still being studied; however, it is believed to modify the brain’s dysfunctional circuits. It can influence the release of neurotransmitters, which are molecules required for communication between brain cells, or it can stimulate underactive areas while inhibiting hyperactive ones.
Parkinson’s disease, essential tremor, dystonia, epilepsy, and obsessive-compulsive disorder have all been successfully treated using deep brain stimulation. When medications and other therapies fail, they provide significant symptom alleviation to many people, thereby improving their quality of life. Despite its intricacy, DBS is regarded as a safe and effective procedure that offers hope to individuals suffering from challenging neurological and mental problems.
3. The Procedure
Typically, the procedure comprises two surgeries:
Lead placement involves using a stereotactic head frame and imaging techniques such as MRI or CT to precisely implant electrodes in the brain. To ensure proper implantation, awake testing may be undertaken throughout the surgery.
Positioning of the Pulse Generator: A small piece of equipment called a pulse generator is put beneath the skin around the collarbone, and cables are introduced to connect it to the brain electrodes.
4. Preparation and Recovery
In addition to adhering to specific pre-surgical instructions, such as fasting and discontinuing certain medications, you will undergo imaging tests to map your brain before surgery. The pulse generator is set up to give personalised stimulation after surgery. Following each surgery, the majority of patients return home the next day after a brief hospital stay to recover.
5. After the Procedure
After Deep Brain Stimulation (DBS) surgery, you may stay in the hospital for a few days so doctors can monitor your condition. Your doctor may also prescribe medicines to help prevent infection and manage pain.
A few weeks after the surgery, you will visit your healthcare provider to activate the pulse generator placed in your chest. The device is programmed from outside the body, and the stimulation level is adjusted based on your needs. It may take several visits over a few months to find the most effective settings.
The device usually works throughout the day, and in some cases, patients may be advised to turn it off at night. The battery of the pulse generator can last several years and can be replaced through a simple procedure when needed.
During recovery, it is important to attend follow-up visits and inform your doctor if you notice symptoms such as fever, severe headache, swelling, weakness, or problems with speech or vision.
Advantages of DBS
Deep Brain Stimulation (DBS) offers several advantages for people with certain neurological conditions. It can help improve symptoms and support a better quality of life.
One major advantage is that DBS can be helpful when medications are no longer effective. In some conditions, medicines may stop working well over time or may cause unwanted side effects. DBS can help control symptoms and may allow patients to reduce their medication dose.
DBS can also reduce symptoms such as tremors, stiffness, and slow movement. This improvement can make it easier for people to perform daily activities and maintain independence.
Another benefit of DBS is that the device can be adjusted. Doctors can change the stimulation settings to find the level that works best for the patient.
In addition, DBS is a reversible treatment. If needed, doctors can remove the device through another procedure. This makes it a flexible treatment option for many patients.
Risks of DBS
Deep Brain Stimulation (DBS) is generally considered safe, but it still carries some risks because it involves brain surgery and an implanted device. The risks may occur during the surgery or after the device is activated.
Surgical risks may include infection, bleeding in the brain, stroke, seizures, or swelling around the brain. Some people may also experience breathing problems, nausea, or temporary confusion after the procedure.
Device-related problems can also occur. These may include movement or incorrect placement of the electrodes, loose or damaged wires, or battery failure. In some cases, another procedure may be needed to fix or replace parts of the device.
Side effects from stimulation may appear when the device is turned on or adjusted. These may include numbness or tingling, muscle tightness, balance problems, speech difficulties, vision changes, dizziness, or mood changes such as depression. Many of these effects improve after doctors adjust the device settings.
Conclusion
DBS helps to treat abnormal neural activity associated with disorders such as epilepsy, dystonia, and Parkinson’s disease by transmitting controlled electrical impulses to specific areas of the brain. DBS is a versatile approach to treating complex neurological problems since it is reversible and configurable, as opposed to traditional operations that permanently alter brain tissues.
Typically, the procedure is carried out in two stages: implanting a pulse generator in the chest and inserting electrodes into the brain. Patients commonly report significant improvements in their quality of life, such as increased motor control, fewer seizures, or relief from obsessive-compulsive behaviours. Although the actual mechanism of DBS is still unknown, research is ongoing to widen its potential applications to encompass additional disorders, making it a realistic option.
Frequently Asked Questions
1. Is DBS a cure for neurological disorders?
DBS is not a cure. The treatment’s purpose is to reduce symptoms while also improving quality of life. It significantly reduces symptoms for the majority of disorders, but it does not treat the underlying ailment.
2. What are the risks associated with DBS?
DBS, like any other operation, carries hazards including brain infection, haemorrhage, and anaesthesia-related issues. Furthermore, there may be side effects such as brief mood swings, tingling, or difficulty speaking, which are often controlled by adjusting the device’s settings.
3. Who is a candidate for DBS?
DBS is typically recommended for persons with symptoms that are difficult to treat with medication or other therapy. To determine their suitability for the procedure, candidates must undergo a thorough screening that includes imaging scans and meetings with specialists.