Small Bowel Transplant
November 5, 2019
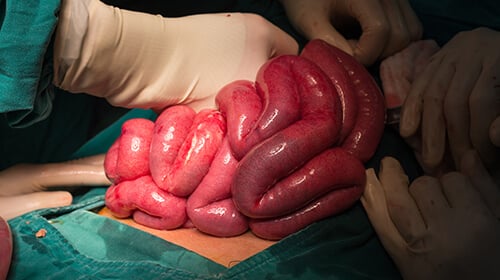
The small intestine is the most important part of the digestive system, as it breaks down food into smaller particles, which the body absorbs to create eneregy. It is also essential for absorption of vital nutrients, minerals and vitamins. Intestinal failure can develop when a person’s small intestine does not provide the necessary long-term nutrition needed to sustain a normal life. This can either happen due to shortening of the intestinal length from previous operations involving removal of large portions of small intestines or due to failure of absorptive mechanisms within the intestine, with a normal length. Intestinal failure leads to need for additional long-term nutrition to be delivered through large veins in the body. This is called ‘total parenteral nutrition’ (TPN).
Patients with irreversible intestinal failure may require all or most of their nutrients and calories through TPN, which is given through catheter placed in the arm, neck, groin or chest. Patients on TPN may live for many years, but long-term use of TPN can result in serious complications, such as repeated infections, clotting of the large blood vessels, electrolyte imbalances, liver damage and micronutrient deficiences. So although TPN sustains life in the short to mid-term, long-term use can lead to various complications, thereby reducing the lifespan of the patient. These TPN feeds are better done at highly specialist hospitals, as they will be more experienced in reducing the risk of line infections and delaying the long-term complications of TPN.
A small bowel (intestinal) transplant is an operation to replace a shrotened or non-functioning small bowel with a healthy bowel from a donor. In some instances, other organs such as liver, pancreas, stomach or large bowel are transplanted along with the small bowel transplant. When the operation involves more than small bowel, it is called as multivisceral transplant (MVT). The liver is included as part of small bowel transplant when there is long-term damage to the liver from the total parenteral nutrition leading to scarring of the liver (fibrosis or cirrhosis). The pancreas is included as it attaches to the small bowel and thereby including it makes the operation technically less challenging. Stomach and large bowel are included depending on if there has been damage to these organs from previous operations the patient might have had.
Small bowel and multivisceral transplant are highy specialised operations that are only carried out in a small number of specialist centres Worlwide. They are not commonly perfomed, although the number of procedures carried out has increased in recent years. The small bowel for transplant mostly comes from the deceased (cadaveric) donor, but needs extensive matching to avoid/reduce the risk of rejection. Hence the waiting time for small bowel transplant can be longer, until which time the patient continues on TPN feeds. In some instances, the small bowel can be obtained from the living donor, but due to the risk to the donor, these are not commonly performed worlwide.
Not all patients with intestinal failure are suitable for small bowel transplant. Due to the complexity of the procedure, only some patients may be considered following a rigorous assessment. The assessment bascially involves review by a multidisciplinary team involving physician, surgeon, anaesthetist, nutrition specialist, endoscopist and others.
The main aim of a small bowel or a multi-visceral transplant is to improve both the quality and the length of patient’s life. Following a successful small bowel transplant, the patient will be able to start eating a week following the transplant, initially in small amounts and subsequently increased depending on the recovery of the transplanted bowel. They will need multiple medications in the initial period, which will reduce over a period of time. The patient will need regular surveillance of their small bowel with endoscopy to ensure there is no rejection. In a minority of patient, the small bowel transplant might not completely make them independent on oral diet, so they may need part of their nutrition through line feeds. Over a period of time, this may change depending on the adaptation of the small bowel.
After the small bowel transplant, the patient will need medications to prevent rejection of the transplanted bowel. These are the immunosuppression medications which reduce the immunity and prevent the body from rejecting the organs. These need to be taken lifelong. Although these medications does add the risk of infections or developing cancers, the risk far outweighs the benefit of living with life threatening intestinal failure and TPN.








